Photodynamic Therapy PDT At A Glance
- Best Results1-2 treatments
- Treatment Recovery2 - 5 days
- Procedure Time45-120 min
- Skin SpecialistDavin Lim
- Duration of Results2-7 years
- AnaestheticNumbing, blocks
- Back to Work1-5 days
- Cost$$
Photodynamic Therapy - PDT
Photodynamic therapy or PDT is a procedure that uses light sensitive chemicals and low-level lasers / Light Emitting Diodes. This treatment can provide limited photo rejuvenation. It is best employed to treat superficial skin cancers, sun damage & sunspots – solar keratosis. I frequently use a combination of fractional lasers & PDT as this combination addresses both pigmentation & cellular damage. Downtime following this procedure ranges between 2 to 5 days.
FactsFacts on PDT / Photodynamic Therapy
- Sun damage can present in many ways including brown liver spots, premature wrinkling, as well as rough dry red and scaly areas on the forehead, nose, cheeks and temples
- The most common form of sunspots are solar keratosis or actinic keratosis
- These sunspots are precancerous and should be treated
- Treatment of background sun damage will enable a Specialist to pick up any cancers at an earlier stage
- PDT combines a light sensitive chemical with radiation of light to destroy abnormal skin cells
- PDT can be effective in treating superficial skin cancers & sun damage, in addition to providing photo rejuvenation
What is PDT or photodynamic therapy?
Photodynamic therapy or PDT is a treatment performed by dermatologists. It uses light sensitive agents combined with oxygen & specific wavelengths of light. This gives a photochemical reaction in the skin killing precancerous & cancerous cells.
PDT is best used for specific management of skin cancers or pre-cancer. It is over-rated for cosmetic indications & is even more over-rated for treating acne (both traditional PDT & the super-expensive Kleresca). Read more to understand.
What skin conditions can be treated with PDT?
PDT is best for treating superficial skin cancers such as basal cell carcinomas, & thin squamous cell cancers known as in-situ SCC/Bowen disease. PDT can also be used to treat sunspots in the form of solar keratosis.

The conditions listed below can also be treated with PDT, however there are better, more effective treatment available-
- Skin rejuvenation: overrated, lasers do a much better job
- Acne: simple creams & peels are more effective in the long run
- Seborrhoea or oily skin; a vitamin A tablet twice a week does a better job
- Sebaceous hyperplasia: lasers offer better results & clearance
- Rosacea: often flares up with PDT, a very small percentage of patients improve
What are the PROS & CONS of PDT?
PDT can be highly effective in the treatment of some forms of skin cancer. Advantages of this treatment include-
PROS
- Precision targeting of lesions
- Less invasive than traditional surgical procedure
- Quick often outpatient treatment
- No long-term side effect
- Excellent cure rate when used correctly
- Minimal scarring post treatment
- Can be repeated on the same sites
- Relatively cost effective
CONS
- PDT only treats superficial skin cancers
- Long term clearance of sun damage is not as good compared to some other treatments
- Relatively expensive compared to cryotherapy (freezing)
- Contraindicated in some forms of blood disorders

Though effective, I prefer to use small spot lasers at 90%+ density to treat sunspots & actinic keratosis. Lasers give excellent outcomes.
How is PDT performed?
There are two ways to perform PDT. Firstly (as described below) is in-clinic application, & secondly (as described later) is at home DIY daylight PDT.
In-clinic PDT is for the management of skin cancers supervised by specialist dermatologists. The process goes something like this-
Step 1: A photosensitising cream is applied to the lesion. To increase absorption of light, some lesion skin may be scraped off prior to application. A comfortable clinic area is provided while the agent is absorbed over a period of 2-3 hours. This allows the cream to be concentrated in the cancer cells.
Step 2: The cream is removed & red light is then delivered over 7 minutes & 30 seconds. The treatment area needs to be protected from light exposure during recovery for at least 48 hours. In some cases, additional treatments are administered during the following weeks or months.
Step 3: The area of treated skin will have some redness, stinging, & peeling. This is entirely normal.
For cases of superficial skin cancers, your dermatologist will arrange a second session 2-12 weeks from the initial. For sun spots, solar keratosis & photo rejuvenation, only one session is required.


View our Treatment Gallery
What is PDT photo rejuvenation & why do I think it is over-rated?
It’s not that it doesn’t work, it is because there are much better options out there. PDT should be employed as a specific treatment as indicated, & not viewed as a ‘what else can we use it for treatment.’ In the context of skin rejuvenation PDT has many limitations including-
- The inability to treat pigmentation & pigmented sunspots
- Minimal to no improvement of wrinkles & fine lines
- Minimal to no dermal remodelling
Better photo rejuvenation treatments include thulium laser resurfacing, BBL & fractional lasers as well as old fashioned Jessner TCA Peels (this works so well!). My main indication for PDT is lesion specific treatment or in the context of reducing solar dysplasia – sun spots in DVA patients.
How long is the recovery period following PDT?
Less than a week in most cases. For small spots including superficial basal cell cancers such as BCCs & IECs you do not require time off work.
For field treatment of sunspots or solar keratosis, recovery takes between 3-7 days. Recovery takes longer with in-clinic illumination compared to DIY daylight PDT. Be guided by your dermatologist.
Off label thulium 1927, one session only. 20mj 22 passes to achieve 92% coverage
.
🔫Laser: Fraxel 1927 in HD or high density settings. At 92% it is still non-ablative
.
👍🏻The wavelength, even with the less ‘powerful’ diode cf. thulium is pretty special. Just finished comparing histology with the 1940 & low & behold it is around 200 microns across the board .. from 3 different laser companies. The dermal remodeling from such superficial penetration is so much more than bulk heating, probably related to cytokine release we have yet to fully understand, same goes to the non selective effects this wavelength has on the vessels 😱😱😱
.
😎Davin Lim
Dermatologist
Brisbane🇦🇺
.
#laserdermatologist #fraxel #fraxeldual #thuliumlaser #laserresurfacing #fractionallaser #laseMd #fraxpro #laserrejuvenation #skinscience
TCA peels are a simple way to rejuvenate skin. This picture is over a decade old, but I still enjoy peels over lasers (more tactile). It’ much like driving a older vintage car, it’s slower to get to your destination but the drive is more enjoyable🚘
.
🔬Skin science: TCA can be applied as a superficial, medium (most common) & deep peel. In this case I employed it as a medium depth peel, to the upper papillary dermis. In some cases I combine it with Jessner for deeper penetration
.
👉Downtime: 5- 8 days depending on the strength and coats
.
😢Pain: Tolerable with topical application of numbing and skin cooling. I do give oral conscious sedation if deeper peeling
.
👍🏻Good for: Skin type 1-2+, pigment, freckles, sun damage, solar keratosis, mild to moderate wrinkles, lentigos/ age spots
.
👎🏼Not good for: Darker skin, deep wrinkles, melasma
.
😎Davin Lim
Dermatologist
Brisbane🇦🇺
#chemcialpeels #TCApeel #jessner #jessnerTCA #skinrejuvenation #skinlightening #skinbrightening #davinlim #dermatology #skinscience
Is PDT painful?
Yes. It can be uncomfortable, especially if we treat large amounts of skin & sun damage. For big cases I normally provide pain relief before illumination of PDT. Daylight PDT is less painful. For in-clinic treatments we use a combination of –
- Oral & injectable sedation & painkillers
- Cryotherapy sprays
- Cooling air
- Short breaks
My nurses will ensure that your treatment is comfortable. Remember if you have pain-relief medication you can not drive for at least 6 hours.
What is daylight photodynamic therapy?
This is a new method of delivering PDT. Some dermatologists use this protocol, others will perform traditional in-clinic illumination. Though the literature supports the use of daylight to illuminate the PDT chemicals (known as ALA or aminolaevulinic acid), most dermatologists (including myself), feel that illumination with low level lasers & light emitting diodes are more effective.
Daylight PDT protocol will differ according to your dermatologist. It goes something like this-
- A photosensitiser agent ( 5-ALA or Metvix) is administered by your dermatologist.
- After washing your face with an appropriate cleanser, a suitable chemical sunscreen will be applied to the treatment areas. Thick scales are removed prior to application. Once the skin is prepped, ALA cream is applied on to the treatment areas.
- You will then go outside for daylight exposure within 30 minutes of application. Daylight exposure will continue for 2-2.5 hours. Do not expose your skin to direct sunlight, sit in the shade. You can take toilet breaks as required.
- After two hours of daylight exposure, remove the residual cream from the treated areas. Wash with Cetaphil cleanser.
- UV exposure should be avoided for 5 days following treatment. Use sunscreen and moisturisers as needed.
- It will take 2-5 days before redness in the treated areas subside.

Daylight PDT is a proven method to reduce sun spots. Super fast healing times, with the convenience of undertaking this procedure at home.
What are the other options available to treat sun damage?
Your dermatologist will discuss other options to treat your sun damage, depending on your downtime, budget & goals. Modalities include-
- Cryotherapy or freezing
- Curettage
- Efudix- 5FU
- Daylight PDT
- Aldara- Imiquimod
- Ablative laser resurfacing
- Fractional laser resurfacing
- Chemical peels
- Retinoids – peels, creams & tablets
Laser resurfacing provides the best cosmesis as it markedly reduces sun damage to both DNA & addresses wrinkles & pigmentation.
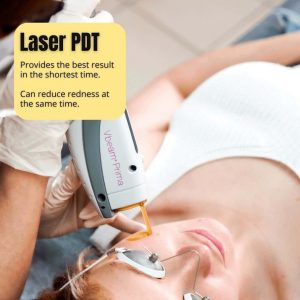
Efudix is the cheapest way to deal with sun spots. It also works very well, however the recovery takes 3 to 4 weeks.
What is the cure rate with photodynamic therapy?
Quoted clearance rates will differ according to which paper you read. It also depends on how you prep the lesions prior to illumination & adjunctive treatments. As a guide-
Superficial cancers including sBCCs & Bowen’s; cure rate ranging between 80-92%. Depends on the site & treatment cycles.
Solar keratosis, remission rates are usually measured at 12 months & range between 70-80+ %.
Does photodynamic therapy treat all forms of skin cancer?
Nope. PDT is only suitable for superficial skin cancers. Your dermatologist will guide you accordingly. Most of us follow these guidelines. PDT is suitable for-
- Superficial basal cell cancers
- IEC or superficial squamous cell cancers
- Sunspots including solar keratosis
PDT is not suitable for pigmented lesions or high-risk basal cell – squamous cell cancers.
What are the side effects of Photodynamic Therapy?
PDT is a relatively safe procedure; however side effects can occur. These include-
Acute pustular reaction (seen in 5% of cases). This is transient & consists of multiple acne like lesions due to massive inflammation. Looks dramatic & scary but settles down within a few days.
Infection; including cold sore virus. This is why we prescribe antivirals to those with a history of cold sores.
Persistent redness, including a flare up of rosacea. Again common, easily manageable with anti-inflammatories & vascular lasers.
Blistering & hyperacute reactions are known to happen. Spectacular, painful but easily managed by your dermatologist.
Spill over reactions occur because the PDT cream seeps from the original site. Ooops. This results in streaky redness as light activates the chemical on normal skin. It will settle down.
Does PDT provide any anti-aging effects?
Yes, it does, especially if combined with lasers. The advantage of PDT is that it treats solar dysplasia or DNA damaged skin via a process called photo rejuvenation. Sun damage can be cosmetic, namely brown spots & dots, red splotchy skin, & broken capillaries. Damage can also lead to abnormal or dysplastic cells.
My usual combination for photo rejuvenation is PDT with activation of low level lasers & fractional laser resurfacing. In some cases, I perform lasers prior to application of PDT as it increases absorption rates of the compound. This is termed laser assisted drug delivery. My combinations include-
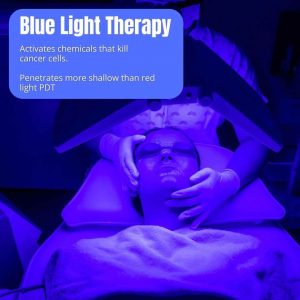
- PDT & LLLT with blue & red light
- PDT & vascular lasers
- Laser assisted PDT with thulium or low density fractional CO2 laser
- PDT followed by 1927 lasers
How much is PDT?
DVA patients: No out of pocket expenses if you hold a Gold or White card for skin.
General population: Single lesion from $350, field treatments from $1290.
Though I perform PDT, my advice is that high density thulium lasers including Fraxel give much better results with less discomfort, downtime & in most cases less expense.
Does medical insurance or Medicare cover PDT?
Medicare does not cover PDT treatment. You may get back a nominal sum from some insurance companies.
The Department of Veteran Affairs or DVA covers PDT for the management of sunspots or solar keratosis, basal cell cancers & other superficial skin cancers. Check if you qualify for this procedure; namely Gold Card holders or White Card for skin associated treatments.
How do you know if PDT is suitable for your skin condition?
Be guided by your dermatologist. Remember, there are many ways to approach skin. Most dermatologists will give you the best options for your skin condition. In some cases, it is PDT, in others simple topicals, tablets, or lasers may be better options.
My most frequently applied indications for PDT is the treatment of superficial cancers, & solar keratosis in DVA patients (as PDT is covered). For general photo rejuvenation, lasers are far more effective, cost effective & less painful than PDT.

Can photodynamic therapy be used to treat acne?
Yup, it sure can. Kleresca is actually PDT. It uses a form of aminolaevulinic acid or ALA & is activated by two wavelengths of blue light. The second wavelength is used as a marketing tool as this is a point of difference compared to normal light sources. PDT can be useful for the management of acne, in particular –
- Patients wanting to spend a lot of money on a trending treatment
- Patients seeking a temporary treatment
- Those who would like to avoid medical treatment
My viewpoint on PDT for acne is that it is a useful modality for select patients. For example, pilots or those who are thinking of joining the aviation industry who are risk averse to the side effects of isotretinoin. Additionally, if isotretinoin is contraindicated, PDT can be a sensible and effective option.
Davin’s Viewpoint on PDT
This is a useful treatment for some forms of skin cancer including low risk basal & superficial SCC in-situ. This especially applies to more cosmetically sensitive sites including the face, chest & decolletage areas. Lesion prep will differ between dermatologists. For younger patients I do not aggressively curette the lesion as this will leave skin colour changes that are often permanent. It is important to note that PDT is only suitable for select cancers. Deeper cancers will require excision.
In the context of field treatments, namely treating the whole (or part) of the face, my main prescription for PDT is daylight PDT as this is more convenient, much less painful & still effective for patients. Though the literature suggest good clearance with daylight PDT, my experience over the past 20 years does not reflect the findings. I prefer a combination of lasers & PDT or high density thulium laser resurfacing over PDT alone.
Lasers offer many advantages over PDT, including the ability to treat dyschromia, namly brown spots & dots (lentigos, pigmented solar keratosis, macular seb keratosis & freckles). Lasers also address solar dysplasia, namely UV induced DNA damage to keratinocytes or skin cells. In the context of comparing PDT to lasers, the latter is also more cost effective, less painful (in the context of illumination), & is associated with a quicker recovery time.
In the context of acne, this procedure has been commercialised by mainstream clinics. The treatment of course is Kleresca. This is essentially PDT that has been marketed to the maximum. The photosensitiser is a porphyrin, the illumination is with blue light, using two spectrums. It can work, but recurrence is the rule. I am very selective as to who I treat (or advice) with Kleresca treatment as this protocol is very expensive.


